*See update on Ollie – May 2021
It had been several weeks of struggling, multiple vet visits, a bout of antibiotics, probiotics, x-rays, nausea shots, and prayer requests that I heard the words “I believe your kitten has megaoesophagus”. Having several special needs cats in our care, and having recently said goodbye to one, my heart sunk into the sole of my shoes as I heard the next steps of bringing in four-month Oliver for a barium scan and how Oliver should be fed and held in an upright position, and this for ten to 20 minutes after he ate. And how rare this disease is in cats; it’s often seen in big dogs like Great Danes. And it’s not a death sentence. With that said, the barium scan confirmed for two days later, I drove back in a daze to break the news to the family.
At this point, I did what most people do – I Googled the disease and searched for support groups on Facebook. The first and most helpful group that I found on Facebook was Feline Megaoesophagus. The members of the group carried us through the most difficult times with encouragement, prayer, and follow-ups. It is a great source of tried and tested advice and knowledge but most importantly it is a place to carry each other’s burdens and share victories and setbacks.
Also, in the desperate search of answers I learnt Megaesophagus is:
…the enlargement of the oesophagus, a muscular tube that runs from the throat to the stomach. The oesophagus functions solely to deliver food from the mouth to the stomach. Megaoesophagus involves a lack of motility required for the movement of food and liquid down to the stomach and can be the result of a variety of underlying diseases or causes.
Petmd.com
To put it in my own words, megaoesophagus is an enlarged oesophagus which causes food and the like not to travel normally down into the stomach. The food remains passive (no peristalsis for those who took biology); this can lead to aspiration and pneumonia (food getting into the lungs), heaving, vomiting and a whole range of secondary issues. Cats can be born with MegaE (hereditary) or it can be acquired (for example: from led poisoning).
So, what does and did this all mean for Oliver? Here is our journey and what helped us along the way.
Symptoms and Diagnosis of MegaE
Initially, we thought Oliver had gastroenteritis (and one vet even believed he was just greedy, guzzling up his food too quickly). He kept vomiting and he couldn’t keep dry food down at all (sometimes not wet food either). After a bout of antibiotics, he did better. But then he started the vomiting again. It wasn’t straight up vomiting either – it was heaving, choking, hiccupping sounds and then after much struggle, he would bring up food. He also made coughing sounds. And he always seemed ravenous and when he did have access to food, he couldn’t stop eating (hence the greedy first diagnosis).
The videos below are two captured to show the vet:
Other Signs

Some of the other signs of MegaE includes anorexia or poor condition, pneumonia, regurgitation, repeated swallowing or gasping of air especially after eating sometimes drinking. On the Facebook support group, some members also said their kittens with MegaE seemed to always be hungry and greedy for food (just like Oliver), while others had zero appetites or interest in food.
Back to the Journey
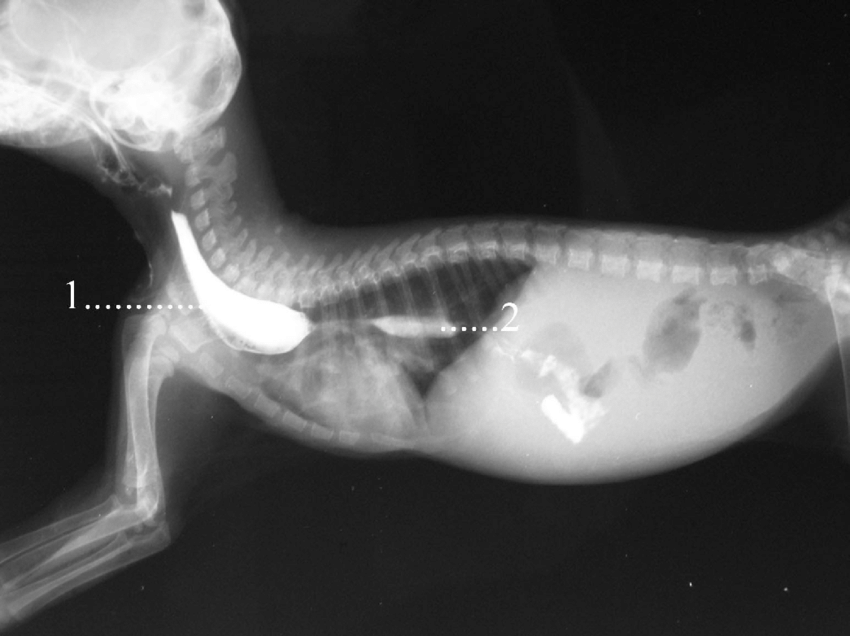
Like I mentioned in the intro, it was a journey to Oliver’s diagnosis. But once the vet suspected MegaE, the first step was a barium scan. Basically, they gave Oliver food laced with barium (which acts like a dye that shows up on scans) and ran scans throughout the day to see (with the dye) how the food moved through his system. After this test was run, the vet confirmed it was MegaE (suspecting persistent right aortic arch/ vascular ring anomaly) and referred us to Onderstepoort. Surgery was the recommendation which we initially did not want to do – we were thousands and thousands of rands out of pocket from the several vet visits and scans, and the cost estimate we received for the surgery was excessive.
But we decided to take Oliver for specialised cat scans to confirm the persistent right aortic arch. More on this later in the blog.
First Steps – The Feeding Regime
Let me digress… as soon as our vet, Dr Elmarie van Tonder, suspected MegaE, she asked us to feed Oliver from an elevated height, and small, liquid meals and then afterwards to hold Oliver up for at least ten minutes, preferably 20 minutes for gravity to do its job. We did this – fed Oliver small tinned fish and mousse with warm water. We tried a raised platform that he initially stood up and ate from. But we then realised it was easier to feed him with a teaspoon from a height (quicker). We then wrapped him in a blankie, set a timer and took him for an upright walk – showing him the garden, or around the house to keep him distracted. This was remarkably effective (he vomited once and that was because he found a bit of kibble his brother dropped inadvertently). But this was also labour intensive – we had to do small meals every two to three hours and then burrito wrap and walk with him. And this is when we realised, we needed to try surgery to attempt to give Oliver a quality life.

The Surgery Journey

We set a date and time for more scans for Oliver at Onderstepoort. The staff were incredibly friendly over the phone, and light-hearted. Something that we needed during a stressful time. We made our appointment, took him in and after many scans were run, the persistent right aortic arch (PRAA)/ vascular ring anomaly was confirmed. The doctor confirmed this is congenital (he was born with it) and that the only way to stop it, is to stop breeding with all the sibling kittens in the litter and the tom and queen that parented the cat.
The vet explained that PRAA happens when the right aortic arch fails to fall away as it would in “normal” cats (or dogs etc), which results in the oesophagus being “entrapped” at the heart base level. So, what happens is that the one part of the oesophagus is enlarged while there is restriction lower down (similar to a funnel – wide at the top and narrow at the bottom). The food sits in the enlarged part which often leads to regurgitation and/or aspiration pneumonia, along with other complications.
Surgery is recommended, especially in kittens and is the only chance to truly ‘fix’, rather than manage PRAA. And with the hope that Oliver could live a normal life, we opted for surgery and a surgeon, Dr Hermien Viljoen was assigned. She spoke to us telephonically and in person. She wanted to make it clear to us that this surgery only had a 50 percent success rate and she wanted us to be cautiously optimistic but understand the odds and that she had lost a kitten last year to PRAA. Dr Viljoen explained that they would put Oliver under anaesthetic and then see if the ring wrapped around the oesophagus is an artery; they would then bind it off/cauterise it and cut it and that was it as far as surgery. He would spend a few days in ICU on morphine; after a few days, tests of him eating without elevation would occur and then it would be home time with aftercare if all went smoothly. She also said there is a chance for kitties to have heart-attacks during surgery but everything would be monitored.
Surgery Day
After surgery day being pushed out by yet another day because more scans had to be conducted, the family were on the edge of their scratch posts. It was tough already because we had to separate the brothers Aslan and Oliver (Aslan being absolutely lost without his brother) and our hearts broke for little Oliver stuck in ICU. But then surgery day, arrived and we were sweating blood, asking for friends to pray for the surgeon and Oliver and peace for us. After two hours of surgery – not because that’s how long the procedure takes but because Dr Viljoen had to keep pausing as the anaesthetist would advise Oliver’s heart rate was too high – it was complete. And the prognosis was good; it looked as though Oliver would recover well.
As straightforward as this sounds now, it was extremely stressful at the time. But through prayer, support and brilliant surgery staff – we made it through.
Post-surgery and After-care

A few days after surgery, Oliver was successfully eating “watered-down” soft food from the ground (not elevated – yay) and not regurgitating. He coughed now-and-then but nothing else and so Onderstepoort said we could fetch our baby, Oliver. With strict feeding instructions, a few syringes of PetCam (pain meds) and stern orders to keep Oliver still while his scar healed (and a “reminder” that he just had major thoracic surgery), we took him home and reunited him with his brother. They hissed at each other – apparently, they didn’t recognise each other after less than a week apart. But after a day – the biggest challenge was to stop the two from rough playing, MMA-fighting and tumble-rumbling like they used to.

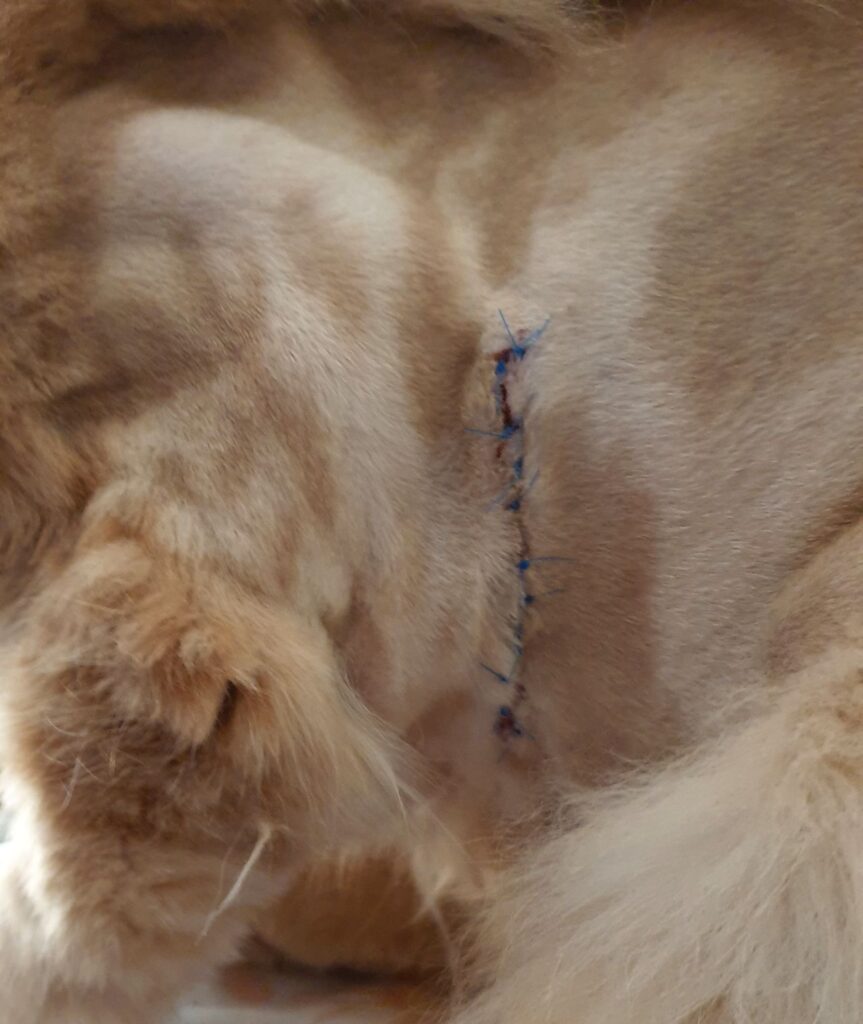
Back to that strict feeding schedule. Post-surgery we received the following feeding instructions:
- Week one and two: small amounts of soft food; every three to four hours fed from the ground (monitoring for regurgitation).
- Week three and four: small amounts of moist/softened kibble every three to for four hours fed from the ground (monitoring for regurgitation).
- Week five and six: gradually transition to larger meals of softened kibble three times a day fed from the ground (monitoring for regurgitation).
- Week seven and eight: gradually transition to a normal diet, feeding two to three times a day fed from the ground (monitoring for regurgitation).
This meant no kibble for at least eight weeks. Unfortunately, Oliver stole some of his brother’s and sisters’ kibble (that was hidden, covered and elevated) about three times over the first few weeks and vomited. Something quite serious for him after the surgery. But fortunately, it didn’t continue, and we became more efficient in hiding the kibble. After about eight weeks post-surgery Oliver will hopefully be able to eat dry food and have a “normal” life. We aren’t there yet (at the time the blog is published). But he is a happy, handsome, active kitten.

The two boys were even recently neutered. They are happy, constantly hungry, growing, loveable and extremely annoying to their older sister “siblings”.

The journey continues but so far it seems all the stress, prayers, funds and sleepless nights were worth it.
The Support and Thanks

During the incredibly difficult times, we had a support network of loved ones praying for us and checking-in constantly. We had the most amazing support from strangers on the MegaE group, Feline Megaoesophagus. And last and not least we had amazing Vets and Vet nurses in our corner. I don’t know all the names but I had it on good authority that Oliver was the darling of Onderstepoort Surgery and our local Vet – this already indicates how invested the staff, students, nurses and doctors are and it was very comforting to know Oliver was adored during times we couldn’t physically be there for him.
Specific thanks should go to Dr Elmarie van Tonder and staff (from Menlyn Animal Clinic) for the diagnosis, check-ins and phone calls – pre/post-surgery. And of course to Dr Hermien Viljoen for her honesty, excellent surgery skills and care of Oliver and Rawden Capell (surgery student), who phoned us several times a day to update us on every detail of Oliver, feeding him every few hours and explaining all the aftercare like a champ – and all the other staff at Onderstepoort who played a role in this journey.
And I truly believe the reason why the surgery and recovery went so well, the surgery bill was so low in the end and that we made it through this trial so triumphantly is because of prayer, miracles and God. All praise be to Him who was and is and is to come!
PS and Other Helpful Tips
Here are some things that helped us through the journey…
Hills and Royal Canin both have mousses and Hills has a gravy; these are easy to water-down and Oliver still loved them (watered-down and all). And it helped us tremendously to have a few of Cosmic Pets playpens (bought from Takealot). We could restrict Oliver post-surgery when he was too boisterous or when we needed to feed the other cats different food.
Update May 2021:
I have been meaning to update this post on how well our Ollie is doing. After following the guidelines and the allotted period of eating only softened food passed, we held our breath as Oliver ate kibble (dry food) freely for the first time since his diagnosis. We watched and feared we were going to hear that all too familiar sound of regurgitation. But it never came. Now, months later Oliver went from our smallest cat to just under 10 kilos (and he is still growing) – beating even his brother who was always double his size. Oliver is a little hoover, and we often have to stop him lovingly bulldozing his brother and sisters who don’t quite eat their allotted mousse or wet food as quickly as he does. He is a bowl cleaner and if he had his way, he would be a Tellytubby (please note we always have pellets out that they can free feed on). The surgery and post-op treatment were, and are a massive success. Oliver is healthy and pretty “normal” (although special) almost like he never had Mega-E. He loves water and baths daily in the communal water bowl/pool (as his horrified siblings watch in severe disdain), he demands being held for at least three hours every day (and tries for more cuddle time) and really is the household darling. But also, he reminds us daily that miracles still happen. Prayers are still answered. And that we have amazing Vets, Vet Nurses, and people in this beautiful country of ours.
PS. The photos say it all (unfortunately some a blurry – but they still tell a beautiful story)

















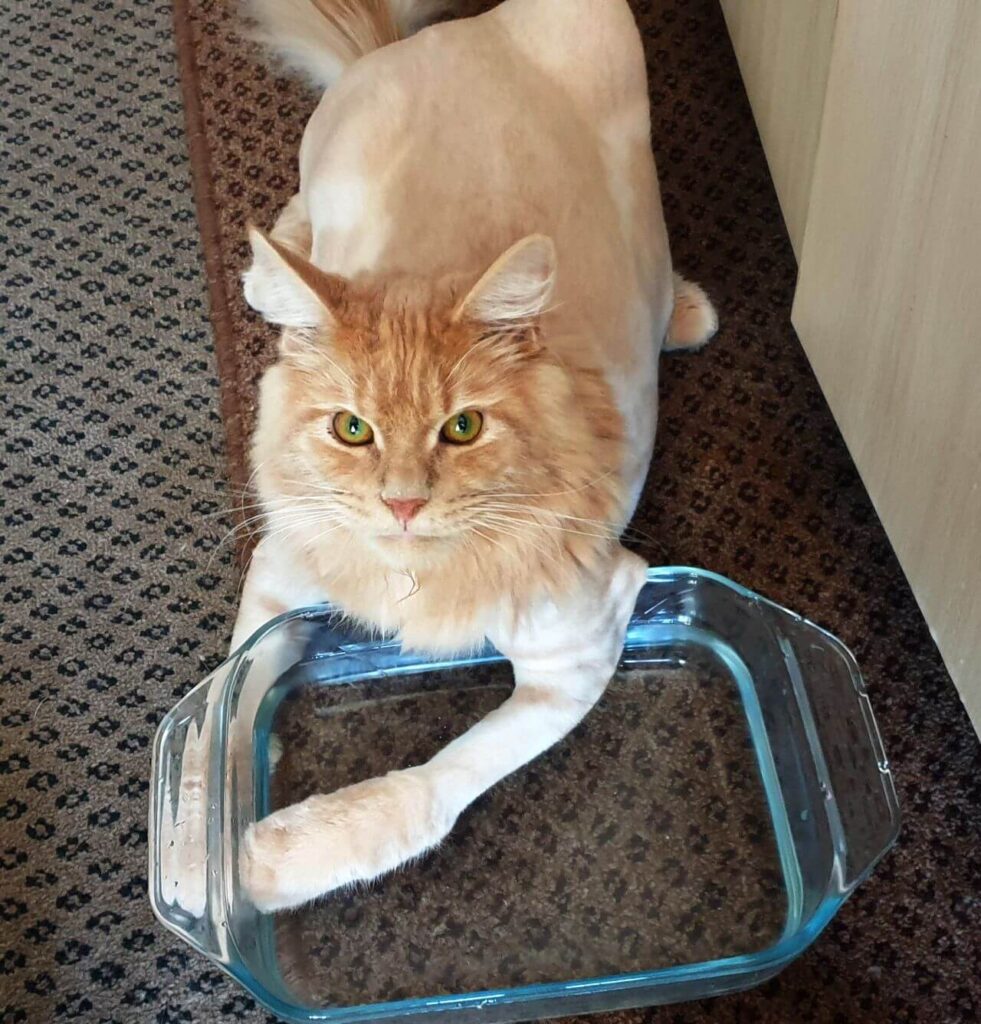







WOW! I came across this and I am delighted that he is doing so well!
Kind regards
Hermien (the very happy veterinarian)
Hi Dr. Hermien.
I am so glad you found us and reached out. We wanted to let you know so many times just how successful your surgery was. We are so grateful to you and your team. I have just added an update to the post at the end. Ollie is like a “normal” very special cat. Just shy of 10 kilos and growing. He is healthy (a little too plump – we are trying to keep him active), happy, and can eat whatever he wants, whenever he wants with no vomiting or regurgitation. Our only struggle with him is transporting him to the vet when we want to groom him (because he is heavy!). He has outgrown his brother and demands cuddles hourly. You have given Oliver a chance at a long and happy life and given us the most precious gift. Thank you. We are forever grateful to you!